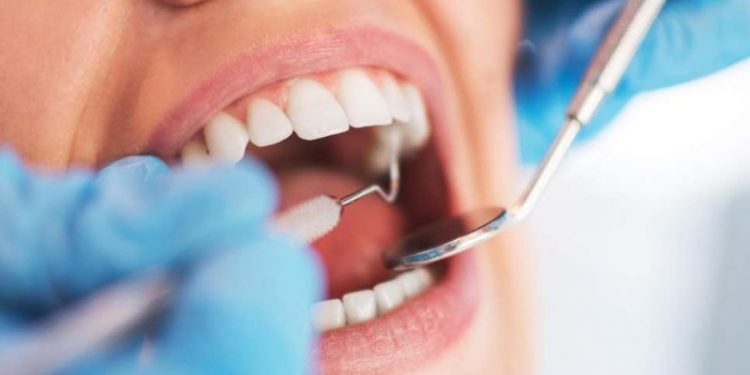
Often everything starts quite harmlessly: with plaque, tartar and the “wrong” bacteria in the mouth. If dental diseases progress, they often rob us not only of nerves and sleep but also of our healthy smiles. Not to mention an unplanned trip to the dentist can prove very costly. Therefore, we want to introduce you to five dental conditions that dentists frequently diagnose, and explain how they arise and how they can be treated.
1. Aphthous ulcers
The term aphthous ulcers describe painful blisters on the gum line, in the oral cavity, on the inside of the lips or on the tongue. From a medical point of view, aphthae are ulcers that can be recognized by a white coating. The small blisters are often disproportionately sensitive to pain for their size and, if they appear on the tongue, for example, they can also affect speaking and eating. Aphthous ulcers on mechanically less stressed areas (e.g., on the inside of the cheek), on the other hand, are usually much less sensitive to pain, but they can interfere with chewing.
Small aphthous ulcers with a diameter of less than one centimetre heal on their own within one to two weeks. With larger aphthae and severe courses, however, it can take weeks to months for the immune system to overcome the pathogen.
2. Gingivitis
Gingivitis is an acute or chronic bacterial inflammation of the gums. Typical symptoms are redness and swelling, pain and an increased tendency to bleeding gums. As with tooth decay, the causes are poor oral hygiene and prophylaxis, because, like tooth decay, gingivitis is also triggered by bacteria that settle on and under the gums. In order to treat gingivitis successfully, the patient must first ensure better oral hygiene. Daily brushing of your teeth, the use of interdental brushes or dental floss and, if necessary, a mouthwash are important prerequisites for bringing the oral flora back into a healthy balance.
Often, however, these measures are no longer sufficient, especially if the gingivitis is already advanced and the gums are already retreating. A professional teeth cleaning at the dentist, during which tartar and other plaque are thoroughly removed, usually ensures that the symptoms subside and a significant improvement within one to two weeks.
On the other hand, if you have a severe form of gingivitis that causes extremely painful and bleeding gums and ulcerations, it can be a sign you need emergency dental services from a reliable dental practice like Mead Dental UK or wherever you may be located. These services are essential as they can help prevent the condition from causing more serious dental problems. If your severe gingivitis isn’t treated right away, it can result in tooth loss and a serious form of gum disease.
3. Calculus Bridge
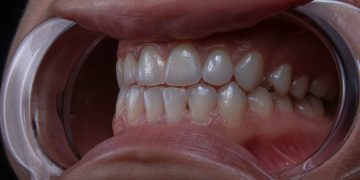
It is a layer of mineralized dead bacteria carrying a small number of minerals containing salivary proteins. It's a hard, bone-like substance that adheres to a person's teeth firmly. Above the gingival margin, it's known as supragingival calculus. The main sign of this type of calculus is a yellow or tan look of the teeth, which occurs in people who fail to eliminate plaque from their teeth. Red and swollen gums, bleeding when brushing, receding gums, constant poor breath, and loose teeth are some of the most common symptoms of calculus bridge and gum disease.
Brushing and flossing your teeth twice a day using a healthy toothpaste is the only method to prevent Calculus Bridge from forming. As we all know, prevention is better than cure, and this is no exception. It is easier to prevent oral problems than it is to cure them. If you take proper care of your teeth, you may never develop Tartar or Calculus that needs to be removed by various dental procedures.
4. Abscesses
An abscess is an encapsulated accumulation of pus in the tissue, which is usually noticeable as painful swelling, in more severe courses also accompanied by fever. Abscesses in the oral cavity are usually caused by pulpitis or tooth root inflammation, triggered by severe caries damage and by bacteria that settle and multiply in gum pockets. Abscesses are also a typical side effect of the development of the wisdom teeth – especially when they cannot break through properly, but rather grow against or under the neighbouring tooth.
Abscesses must be treated by a dentist, who first clarifies the exact cause as part of an examination, possibly with an X-ray. The abscess filled with pus must then be surgically opened and drained. This is usually done with a local anaesthetic and is therefore painless for the patient. If the abscess is open, the dentist can drain the pus and then rinse the wound to remove any debris. In severe cases, an antibiotic can be administered locally, usually in the form of a gel, which is applied directly to the affected area.
5. Cysts in the jaw
Like abscesses, jaw cysts are encapsulated cavities in tissue that are usually filled with fluid. Unlike abscesses, which are always filled with pus, cysts can contain both pus and blood or sebum. In addition, both differ in their delimitation from the surrounding tissue, because cysts have a visible covering layer (epithelium), while abscesses merge seamlessly into healthy tissue.
This difference is also responsible for the fact that ectopy is usually performed on a cyst; the cyst is surgically removed. The remaining cavity is then filled with a bone substitute by the oral surgeon and the wound is then sutured. Only in cases in which a cystectomy is not possible (such as a cyst that has formed around the roots of a tooth worth preserving) is the cyst surgically opened like an abscess so that the fluid can escape. Then by inserting a so-called “obturator” Keeps the cyst open and prevents the early closure of the wound, so that the bone has enough time to renew itself from the inside and to close the cavity.